Peritoneal Dialysis PD
bloodless, painless, freedom, gentle...
PERITONEAL DIALYSIS or PD:
Here are few links and articles that are a necessity for all new patients to PD.
Treatment Choice: Peritoneal Dialysis
Peritoneal dialysis is another form of dialysis that removes wastes, chemicals, and extra water from your body. This type of dialysis uses the lining of your abdomen to filter your blood. This lining is called the peritoneal membrane and acts as the artificial kidney.
How Peritoneal Dialysis Works
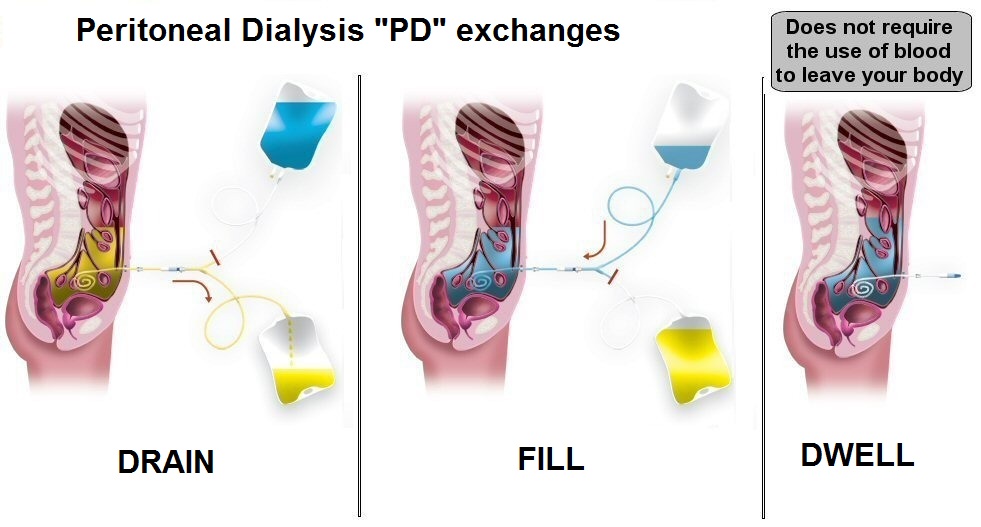
A solution of minerals and sugar (dextrose) dissolved in water, called dialysis solution, is transported through a catheter into your abdomen. The sugar concentration in the dialysis solution draws out the excess water, wastes, and chemicals from the tiny blood vessels in your peritoneal membrane. After several hours, this solution is drained out of your abdomen through the tube, the peritoneal dialysis catheter (PD catheter), taking the wastes from your blood with it. The process is repeated by refilling your abdomen with fresh dialysis solution, and this cycle is called an exchange. There is another type of sugar called icodextrin, is now being used in special conditions where removing excess fluid is challenging.
Getting Ready, preparing for peritoneal dialysis
Before your first treatment, a surgeon will implant a catheter into your abdomen.
It is important to allow adequate time, usually 3–6 weeks, for the insertion site to heal. Planning your dialysis access can improve treatment success. This catheter is permanent to help transport the dialysis solution to and from your abdomen during treatment.
Types of Peritoneal Dialysis
There are four types of peritoneal dialysis available.
(1) Continuous Ambulatory Peritoneal Dialysis (CAPD)
CAPD is a form of peritoneal dialysis that does not require a machine and can be done in any clean, well-lit place. During CAPD, your blood is continuously being cleaned using a dialysis solution that passes from a plastic bag through the peritoneal dialysis catheter into your abdomen, where it stays for several hours with the catheter sealed. This time period is called the “dwell time”. Afterwards, you drain the used dialysis solution into an empty bag for disposal and refill your abdomen with fresh dialysis solution to begin the cleaning process again. CAPD usually involves a dwell time of four to six hours or more, and the process of draining the and refilling takes about 30–40 minutes. Most people change the dialysis solution at least four times a day and sleep with solution in their abdomens at night. With CAPD, there is no need to wake up during the night up to perform the dialysis tasks.
(2) Continuous Cycler-assisted Peritoneal Dialysis (CCPD) (the ideal type)
CCPD utilizes a machine known as THE CYCLER, that fills and empties your abdomen three to five times while you sleep at night. In the morning, you begin a single exchange that remains in your abdomen the whole day. Additionally, you may perform another exchange in the middle of the afternoon without the cycler to enhance the waste removal and to reduce the leftover fluid in your body.
(3) Combination of CAPD and CCPD
If your peritoneum filters the wastes slowly, or if you are a large person, you may require a combination of CAPD and CCPD to achieve the adequate dialysis dose. For instance, some individuals may use a cycler at night and perform one exchange during the day. Others may do four exchanges during the day and use a mini cycler to perform one or more exchanges during the night. Your health care team will collaborate with you to determine the optimal routine.
(4) Intermittent Peritoneal Dialysis (IPD)
Intermittent exchanges are mostly used in the hospital setting for acute kidney failure.
Who Performs Peritoneal Dialysis
Both types of peritoneal dialysis, CAPD and CCPD, are usually performed by the patient without assistance from a partner. CAPD is a type of self-treatment that does not require a machine. On the other hand, with CCPD, a machine is needed to drain and refill your abdomen.
Possible complications of peritoneal dialysis
Peritonitis, a serious abdominal infection, is the most common problem associated with peritoneal dialysis. This infection can occur if the opening where the catheter enters your body becomes infected, or if contamination occurs during the connection or disconnection of the catheter from the bags. Peritonitis treatment requires antibiotic prescribed by your nephrologist.
To prevent peritonitis, it is crucial to strictly follow the procedures and learn to recognize the early signs of peritonitis, such as fever, unusual color or cloudiness of the drained peritoneal dialysis fluid, and redness or pain around the catheter. If you notice any of these signs, notify your doctor or nurse right away so that they can quickly treat the peritonitis to avoid further complications.
Diet for peritoneal dialysis
A peritoneal dialysis diet is slightly different from an in-center hemodialysis diet.
(1) You will still need to limit salt and liquids, but you may be able to consume more of each compared to the in-center hemodialysis diet.
(2) You must consume more protein.
(3) You may have different restrictions on potassium. You may even need to consume high-potassium foods.
(4) You may need to reduce the number of calories you consume because there are calories in the dialysis fluid that may cause weight gain.
(5) Your doctor and a dietitian who specializes in helping people with kidney failure will be able to assist you in planning your meals.
Advantages and disadvantages of different type of peritoneal dialysis
Each type of peritoneal dialysis has advantages and disadvantages.
CAPD
Advantages
+ You can do it alone.
+ You can perform the required number of exchanges each day at times you choose.
+ You can do it in many locations.
+ You don’t need a machine.
+ You won’t experience the ups and downs that many patients on hemodialysis feel.
+ You don’t need to travel to a dialysis center three times a week.
Disadvantages
– It may disrupt your daily schedule.
– It is a continuous treatment, and all exchanges must be performed seven days a week.
CCPD
Advantages
+ You can do it at night, mainly while you sleep.
+ You are free from performing exchanges during the day.
Disadvantages
– You need a machine.
– Your movement at night is limited by your connection to the cycler.
Working with Your Health Care Team
Questions you may want to ask:
-
Is peritoneal dialysis the best treatment choice for me? If yes, which type is best and why?
-
How long will it take me to learn how to perform peritoneal dialysis?
-
What does peritoneal dialysis feel like?
-
How will peritoneal dialysis affect my blood pressure?
-
How will I know if I have peritonitis, and how is it treated?
-
As a peritoneal dialysis patient, will I be able to continue working?
-
How much exercise should I engage in?
-
Where do I store my supplies?
-
How often will I see my doctor?
-
Who will be on my health care team, and how can they help me?
-
Whom should I contact with problems?
-
Who can I talk about finances, sexuality, or family concerns?
-
How and where can I communicate with other people who have faced this decision?
Peritoneal Dialysis is Not a Cure
Peritoneal dialysis is a treatments that help replace the functions of your kidneys. These treatments help you feel better and live longer, but they do not cure kidney failure. Although patients with kidney failure are living longer than ever before, kidney disease can cause problems such as heart disease, bone disease, arthritis, nerve damage, infertility, and malnutrition over time. These problems will not go away with dialysis, but doctors now have new and improved ways to prevent or treat them. You should discuss these complications and their treatments with your doctor.
SPECIALTIES
PHYSICIANS RESOURCES
SERVICES
CONTACT US