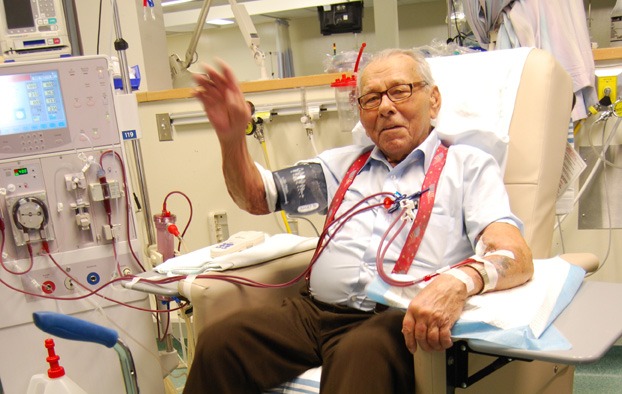
Hemodialysis HD
The most common modality for renal replacement therapy, "DIALYSIS THROUGH THE BLOOD"
Here are a few links and articles that are a necessity for all new patients to Hemodialysis.
-
GO ahead and have your Hemodialysis access, preferably a native AV Fistula, placed as early as recommended by your physician. There is plenty of evidence to support that:
Treatment Choice: Hemodialysis
Hemodialysis is a medical procedure that utilizes a machine to effectively cleanse and filter your blood, eliminating harmful wastes, excess salt, and additional fluids. By undergoing hemodialysis, you can maintain your blood pressure and achieve a balanced level of essential elements like potassium, sodium, calcium, and bicarbonate.
In case of kidney failure, hemodialysis serves as a reliable means of replacing some of the functions of your kidneys. However, additional measures such as dietary regulations, fluid intake limits and medications may also be required. The specifics of your dietary needs, fluid intake, and medication requirements will depend on the treatment option you choose, in consultation with your healthcare provider.
How Does Hemodialysis Work?
Hemodialysis involves the use of a specialized filter called a dialyzer, which acts as an artificial kidney to clean your blood. The dialyzer is a cylinder connected to the hemodialysis machine.
During the hemodialysis treatment, your blood transported through a series of tubes and into the dialyzer, where it is cleansed of waste products, excess salts and additional water. The purified blood is then directed back into the body through another set of tubes. The hemodialysis machine continuously monitors the blood flow and eliminate waste products from the dialyzer.
Typically, hemodialysis is carried out three times a week, each session lasting from three to five hours or more. During the treatment, you are free to read, write, sleep, talk, or watch TV, making it relatively a comfortable experience.
Getting ready, preparing for hemodialysis
In the months leading to your first hemodialysis treatment, an access to your bloodstream will need to be created. This surgical procedure may require a hospital stay overnight, but many patients may undergo the procedure as outpatient. This access is crucial in allowing for the efficient transportation of blood to and from the dialyzer, without causing any discomfort. There are two primary types of access available: a fistula and a graft.
—-Arteriovenous fistula, AVF, is the best choice
A surgeon creates this by utilizing your own blood vessels, connecting an artery directly to a vein, typically in your forearm. The increased blood flow causes the vein to grow larger and stronger, making it suitable for repeated needle insertions. Although this kind of access is the best option, it may take several months to mature and become ready for use.
—-Arteriovenous Graft, AVG
A graft is a synthetic tube that connects an artery to a vein, unlike an AV fistula, it does not require the same time to develop, so it can be used sooner after the placement. However, a graft is more likely to have problems with infection and clotting.
—-Catheter for temporary access, Permacath
If your kidney disease has progressed rapidly, you may not have enough time to establish a permanent vascular access before starting hemodialysis treatment. In this case, you may need to use a temporary catheter, a small, soft tube inserted into a vein in your neck, chest. Some people use a catheter as a long-term access. However, catheters that will be needed for more than two weeks are designed to be placed under the skin to improve comfort and reduce complications.
Who performs the hemodialysis treatment?
Hemodialysis is typically performed at a dialysis center by patient care technicians (PCT) who work under the supervision of nurses.
If you opt for in-center treatment, you will have a set time slot three times a week usually on Monday, Wednesday, and Friday or Tuesday, Thursday, and Saturday. In case you do not get the desired time slot initially, you can request to be put on a waiting list for the preferred time. Additionally, you may be able to switch time with another patient for a special event.
Some centers offer in-center nocturnal hemodialysis, which involves a longer treatment period during the night while you sleep at the center.
The treatment allows for more dialysis, resulting in fewer dietary and fluid restrictions, and it frees up your days for work, child care, hobbies, or other activities.
You also have the option to learn how to perform hemodialysis treatments at home. When you are the only patient, it is possible to undergo longer or more frequent dialysis, which comes closer to replacing the steady work of healthy kidneys. Daily home hemodialysis (DHHD) involves five to seven treatments per week, lasting for two to three hours at a time, and can set the schedule according to your preferences. If your health plan covers more than three treatments, you could opt to do shorter treatments in the mornings or evenings.
Nocturnal home hemodialysis (NHHD) is performed three to six nights per week while you sleep. Either DHHD or NHHD will allow for a more normal diet and fluid intake, with fewer blood pressure and other medications.
Many programs involve people receiving hemodialysis at home with the assistance of a trained partner. Learning to do home hemodialysis is similar to learning to drive a car. It may be intimidating at first, but with a few weeks of training, it becomes routine. The dialysis center provides the machine, training, and 24-hour support in case of any questions or problems. The new machines for home dialysis are smaller and more user friendly than the ones used in the center.
There are multiple dialysis centers to choose from in most towns, providing you with the opportunity to select one that suits your needs. You can visit these centers to determine if they offer the treatments you require or a suitable time slot available. Depending on the center, you may be able to use your laptop or cell phone, or have visitors during the session. However, some centers may have restrictions on these activities.
If you opt for in-center treatment, it may be preferable to choose a center near your home to minimize travel time. On the other hand, if you chose to do home treatment, you only need to visit the center once a month after completing your training. Consequently, you can choose a center that is further away, if you are comfortable with traveling once a month.
Possible complications of hemodialysis
Among individuals undergoing hemodialysis, hospitalizations due to vascular access problems is the most frequent occurrence. Typical issues include infection, clotting, and insufficient blood flow. These problems can cause your treatments to stop working. As a result, multiple surgeries may be necessary to establish a properly functioning access.
Rapid changes in the body’s water and chemical balance during hemodialysis treatment can result in additional problems. Two common side effects, muscle cramps and hypotension, a sudden and significant drop in blood pressure that may cause weakness, dizziness, or nausea.
Typically, a few months are required to adapt to hemodialysis, and side effects can often be promptly and efficiently treated by reporting them to your physician and dialysis staff. You can minimize the likelihood of side effects by following a proper diet, regulating your liquid intake, and adhering to medications instructions.
Diet for hemodialysis
Hemodialysis along with a proper diet, can help reduce the accumulation of wastes in your blood. A dietitian is available at all dialysis centers to assist you in planning meals according to your doctor’s orders. When selecting foods, Keep in mind:
(1) Eat balanced amounts of high-protein foods such as meat, chicken and fish.
(2) Control your intake of potassium. This mineral is found in salt substitutes, some fruits (such as bananas and oranges), some vegetables, chocolate, and nuts. Consuming too much potassium can be dangerous to your heart.
(3) Limit your fluids intake. When your kidneys are not functioning, fluids can quickly accumulate in your body causing your tissue swelling and potentially leading to high blood pressure, heart problems, cramps, and low blood pressure during hemodialysis.
(4) Avoid salty foods, which can make you thirsty and lead to fluid retention in your body.
(5) Restrict your intake of foods such as milk, cheese, nuts, dried beans, and dark colas, as they contain large amounts of phosphorus. Too much phosphorus in your blood causes calcium to be pulled from your bones, resulting in weakened and brittle, which may lead to arthritis. To avoid bone problems, your doctor may prescribe special medications called phosphate binders, which you must take with meals every day as directed.
Advantages and disadvantages for different hemodialysis modalities
Each person responds differently to similar situations, so what may be a negative factor for one person could be a positive one for another. Below is a list of the general advantages and disadvantages of in-center and home hemodialysis.
In-center Hemodialysis
ADVANTAGES:
+ Dialysis facilities are widely available.
+ Trained professionals are available to help you at all times.
+ You can interact and socialize with other patients.
+ You do not need a partner to help you with treatment, and you don’t need to keep equipment at home.
DISADVANTAGES:
– Treatments schedules are predetermined by the center and are relatively inflexible.
– You need to travel to the dialysis center for treatment.
– This treatment modality requires the strictest diet and fluid limits.
– You will need to take and pay for more medications.
– You may experience more frequent ups and downs in how you feel on a day-to-day basis.
– It may take a few hours to feel better after a hemodialysis treatment.
Home Hemodialysis
ADVANTAGES:
+ You can do it whenever you choose, but as often as your doctor orders.
+ You don’t have to travel to a dialysis center.
+ You’ll feel more independent and in control of your treatments and life.
+ New portable machines require less space and may go on travel.
+ You’ll experience fewer ups and downs in how you feel day-to-day.
+ Home hemodialysis is more work-friendly than in-center treatment.
+ Your diet and fluids will be much closer to normal.
+ You can spend more time with your loved ones.
+ Better cardiovascular outcomes, better quality of life, and better survival.
DISADVANTAGES:
– You must have a partner to help you.
– your family may feel stressed helping you with treatments.
– You and your partner need training.
– You need space for storing the machine and supplies at home.
– You may need to take a leave of absence from work for training.
– You’ll need to learn how to insert the dialysis needles into the hemodialysis access.
– Daily and nocturnal home hemodialysis are not yet offered at all locations.
Working with Your Health Care Team
Here are some questions you may want to ask:
-
Is hemodialysis the best treatment choice for me? Why?
-
Can I choose the dialysis center I want to go to?
-
What should I consider when choosing a dialysis center?
-
Will my kidney doctor see me at the dialysis center?
-
What does hemodialysis feel like?
-
What is self-care dialysis?
-
Is home hemodialysis available in my area? How long does it take to learn? Who will train me and my partner?
-
which type of hemodialysis access is best for me?
-
Can I continue to work while on hemodialysis? Can I have treatments at night?
-
How much exercise should I do?
-
Who will be on my health care team? How can they help me?
-
Who can I talk about finances, sexuality, or family concerns?
-
How/where can I talk with other people who have faced this decision?
Hemodialysis is Not a Cure
Hemodialysis is a treatment that help replace the functions of your kidneys. These treatments help you feel better and live longer, but they do not cure kidney failure. Although patients with kidney failure are living longer than ever before, kidney disease can cause problems such as heart disease, bone disease, arthritis, nerve damage, infertility, and malnutrition over time. These problems will not go away with dialysis, but doctors now have new and improved ways to prevent or treat them. You should discuss these complications and their treatments with your doctor.
SPECIALTIES
PHYSICIANS RESOURCES
SERVICES
CONTACT US